
Ever read your medical record? Here’s why you should

Do you ever read the notes written by your doctor or health practitioner during a medical visit? If not, you might want to check them out. Usually, these medical notes are full of helpful insights about your health and reminders of recommendations discussed. And there’s medicalese, of course: hard-to-pronounce illnesses, medications, and technical terms.
But you may be surprised to see incorrect information or unexpected language, tone, or even innuendo. Was your past medical history really that “unremarkable”? Did you actually “deny” drinking alcohol? Did the note describe you as “unreliable”?
Here’s how to decipher unfamiliar lingo, understand some surprising descriptions, and flag any errors you find.
What’s in a medical note?
A standard medical note has several sections. These include
- a description of current symptoms
- past medical problems
- a list of medications taken
- family medical history
- social habits such as smoking, drinking alcohol, or drug use
- details of the physical examination
- test results
- a discussion of the big picture, along with recommendations for further evaluation or treatment.
Notes tend to be more complete for a new patient or annual exam. Follow-up notes may not cover all of these points.
What’s potentially confusing about medical notes?
Most medical notes aren’t written using plain language because they aren’t intended primarily for a nonmedical audience. So it’s common to run across:
- Medical jargon: You had an upset stomach and a fever. Doctors may say “dyspepsia” (upset stomach) and “febrile” (fever).
- Complicated disease names: Ever heard of “multicentric reticulohistiocytosis” or “progressive multifocal leukoencephalopathy?” These are just two of thousands of examples.
- Use of common language in uncommon ways: For example, your medical history might be called “unremarkable” and test results called "within normal limits” rather than “normal.”
- Abbreviations: You might see “VSS” and “RRR,” meaning “vital signs stable” with a pulse that has a “regular rate and rhythm.”
If you’re having trouble deciphering a note or understanding your health issues, tests, and recommendations, check in with your doctor’s office for clarifications. The more you understand about your health and your options for care, the better.
What if a medical note is incorrect?
Minor errors in medical notes are not rare: maybe you had your tonsils removed 30 years ago, not 10 years ago. But there can be more important errors: stating that arthritis in your left knee is severe when it’s actually the right knee that’s severe could lead to having x-rays (or even surgery!) on the wrong side. And not properly recording a family history of cancer or heart disease could mean missing out on timely screening tests or preventive treatments.
In an era of ever-increasing time pressure, use of voice recognition software, electronic record templates, drop-down menus, and ability to copy and paste text, it’s easier than ever for health care providers to make (and perpetuate) errors in the medical record.
If you do see an important error that could affect your health, ask your provider to amend it.
What if the language in a medical note seems offensive?
Numerous studies have highlighted the problem of stigmatizing language in medical notes that can leave people feeling judged or offended. Negative attitudes can affect the quality of our health care and willingness to seek care, and can also widen health disparities. One study linked stigmatizing language to higher rates of medical errors. Of note, this study found higher rates of stigmatizing language and medical error among black patients.
Examples include:
- Depersonalization: A note might describe a patient as “a drug abusing addict” rather than a person struggling with drug addiction.
- Insulting or inappropriate descriptors: Notes might contain subjective descriptions that paint the patient in an unflattering light without providing context. For example, the note might say “the patient is unkempt and is drug-seeking” rather than “the patient is experiencing homelessness and has severe, chronic pain.” If a person’s recall of medical events from the past is hazy, they may be called “unreliable.”
- Dismissiveness: A medical note may suggest a symptom is not real or is exaggerated, rather than taking the complaint seriously.
- An untrusting tone: Language such as “she claims she never drinks” or “he denies alcohol use” may suggest mistrust by the physician.
Why might this happen, anyway?
How does such language make its way into medical notes? (To be clear, these possible explanations are not justifications.)
- Tradition and training: Medical trainees, like other learners, tend to follow the lead of their mentors. So if stigmatizing language is used by an instructor, trainees may do the same.
- Time pressure: With medical documentation (as in most everything else), mistakes are more common if you’re rushing.
- Bias: Like everyone else, doctors have biases, including ones they aren’t aware of. How we are taught to think about people — by family, by society — can spill over into every area of life, including work.
- Frustration: Doctors may feel frustrated by patients who don’t follow their recommendations. That frustration can be reflected in their medical notes. For example, a note may say, “As expected, the patient’s blood sugar is high; he is still not checking his blood sugar or following the diet recommended by his nutritionist.”
If the language in a note is confusing or bothersome, ask about it. The Open Notes movement and federal legislation have given most of us much better access to our medical records. This has worthy goals — greater transparency and better communication with people about their medical care — and unintended consequences.
Is changing language in notes that health practitioners once shared mainly with each other a positive consequence? Mostly. Yet some doctors worry that notes will become less specific, accurate, or useful since they may leave out information that might upset a patient.
The bottom line
I encourage you to read your health providers’ notes about your care. If there is a substantial error or something you find confusing or objectionable, ask about it. By the way, a signed medical note cannot usually be revised. However, your doctor can make clarifications or correct mistakes in an addendum at the end of the note.
As more and more patients read their medical notes, it’s likely that health providers will be more conscientious about the language they use. So, wide access to medical notes may improve not only people’s understanding of their health, but also the quality of notes over time.
It's worth remembering that the medical note is not the most important thing that happens during a visit to your doctor. A great note isn’t the same as great care, and vice versa. Still, your medical notes can be a valuable source of health information that differs from all others, including trusted health sites and social media: they’re written by your doctor and they’re all about you.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD

Dog bites: How to prevent or treat them
 Each year, more than 4.5 million dog bites occur in the United States. Despite what you might assume, most of these incidents don’t happen when an unfamiliar dog attacks someone in a park or another outdoor location. Instead, most dog bites are inflicted by a pet dog in a home.
Each year, more than 4.5 million dog bites occur in the United States. Despite what you might assume, most of these incidents don’t happen when an unfamiliar dog attacks someone in a park or another outdoor location. Instead, most dog bites are inflicted by a pet dog in a home.
Here’s advice for avoiding these upsetting and potentially serious injuries — and the steps you should take if you sustain a dog bite.
Why do dog bites happen?
Some dog bites happen by accident when people wrestle or play tug-of-war with their dog. But most of the time, dogs bite people as a reaction to feeling stressed, threatened, scared, or startled, according to the American Veterinary Medical Association (AVMA). More than half of dog bites occur in children, and they’re far more likely to be seriously injured than adults.
“People don’t always heed the behavioral signals that a dog is uncomfortable,” says Dr. Christopher Baugh, associate professor of emergency medicine at Harvard Medical School. For example, some dogs are highly territorial and will bark, growl, snap, and lunge if outsiders enter their space — whether that’s an apartment, yard, or crate. Or dogs may exhibit resource guarding, which shows up as anxious, aggressive behavior around food, toys, or beds.
“These situations can be high-risk, and children in particular have less awareness of that risk,” says Dr. Baugh, who has children and two mixed-breed rescue dogs, Harley and Roxi.
What can you do to prevent dog bites?
Any dog — even a sweet, cuddly dog — can bite if provoked, according to the AVMA. Never leave young children alone with a dog without adult supervision. And teach children to never disturb a dog while it’s eating, sleeping, or caring for puppies.
In a study of 321 facial dog bites treated at Harvard-affiliated Massachusetts General Hospital over a 20-year period, 88% of the bites were from known dogs. Most were in adults and occurred after playing with the dog, feeding the dog, and placing their face close to the dog. However, the hand (usually a person’s dominant hand) is probably the most common location for a dog bite in an adult, says Dr. Baugh.
Other tips from the CDC to prevent dog bites include the following:
- Always ask a dog’s owner if it’s okay to pet their dog, even if the dog appears friendly.
- Make sure the dog sees and sniffs you before reaching out to pet it.
- Don’t pet a dog that seems to be hiding, scared, sick, or angry.
What if an unfamiliar dog approaches you? Remain calm and still, avoiding eye contact with the dog. Stand with the side of your body facing the dog and say “no” or “go home” in firm, deep voice. Wait for the dog to retreat or move yourself slowly away.
What should you do if you’re bitten by a dog?
Clean the wound with mild soap and running water, then cover it with a clean bandage or cloth. Some online resources recommend applying an antibiotic ointment or cream. But these products are recommended only for people with clear evidence of an infection, such as redness, pus, pain, swelling, or warmth, according to the American Academy of Dermatology.
If the injury is serious — with a bite on the face, heavy bleeding, or a possible broken bone — go to the emergency room. That’s also a good idea if you’re bitten by an unknown or stray dog, in the rare event that you might need medicines to prevent rabies (rabies post-exposure prophylaxis).
“Often, people are shocked after being bit and will understandably focus all their attention on their wound,” says Dr. Baugh. The dog’s owner may check in to see if you’re okay, but then walk away. But you should get the person’s contact information and make sure the dog is vaccinated against rabies, he says.
Keep in mind that:
- Emergency rooms are often crowded with long waits, so an urgent care clinic is a good option if the injury doesn’t require immediate attention.
- Some wounds require stitches, ideally within 12 to 24 hours.
- The doctor may prescribe antibiotics to prevent possible infections, especially if you have health problems such as a weakened immune system or diabetes.
- You may also need a tetanus booster if you haven’t had one in the past 10 years. If your vaccine history isn’t available or you can’t remember, you’ll get a tetanus booster just in case.
What if a dog bite is less serious?
Let’s say you have a less serious bite from a family dog known to have a current rabies vaccine. Bites that don’t require stitches can be cleaned with mild soap and running water, then evaluated by your regular health care provider. They may tell you to simply monitor the wound for signs of infection.
“Doctors are trying to be more thoughtful about prescribing antibiotics and limit their use in low-risk situations, because overuse contributes to antibiotic resistance and exposes people to potential side effects without any benefit,” says Dr. Baugh.
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
Julie Corliss is the executive editor of the Harvard Heart Letter. Before working at Harvard, she was a medical writer and editor at HealthNews, a consumer newsletter affiliated with The New England Journal of Medicine. She … See Full Bio View all posts by Julie Corliss
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD
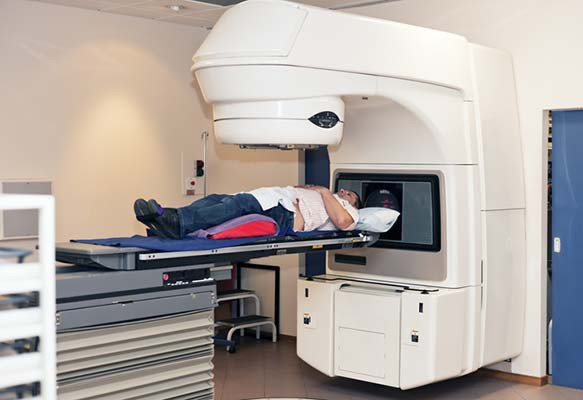
Prostate cancer: Brachytherapy linked to long-term risk of secondary malignancies

When cancer patients are treated with radiation, it’s possible that the therapy itself may cause new tumors to form in the body later. Radiation kills cancer cells by damaging their DNA, but if the treatments cause genetic damage to normal cells near the radiation target, there’s a small risk that these secondary malignancies may arise over time.
Just over 10 years ago, Canadian researchers set out to assess the risk of secondary malignancy among men with prostate cancer who were treated with a type of radiation called brachytherapy. Unlike radiation delivered from sources outside the body, brachytherapy is accomplished by implanting dozens of radioactive pellets, or “seeds,” directly into the tumor site. Those seeds, which are never removed, emit radiation at a dose that declines toward zero over the course of a year.
Brachytherapy has the advantage of convenience. Instead of traveling for repeat sessions of radiation, men need only one treatment, usually given in an outpatient setting. But brachytherapy is also falling out of favor, in part because newer types of external beam radiation deliver high-precision doses with fewer side effects.
Study methodology and results
The Canadian study compared rates of secondary malignancies in the pelvis among men treated either with brachytherapy or with surgery to remove the prostate. All the treatments took place in British Columbia between 1998 and 2000. The brachytherapy group included 2,418 men with an average age of 66, while the surgically-treated group contained 4,015 men whose average age was 62. Within that group, 2,643 men had been treated with surgery alone, and 1,372 men with surgery plus external beam radiation given later.
After median follow-ups of between 5.8 years (brachytherapy) and 6.4 years (surgery), the study team reported in 2014 that there was no difference in rates of secondary malignancies between the groups, or with cancer incidence in the general population.
But that’s no longer the case: In April 2024, the researchers published updated findings. This time, rates of new cancers in the pelvis — including the bladder and rectum — were higher in the brachytherapy group. Specifically, 6.4% of brachytherapy-treated men had secondary malignancies at 15 years of follow-up, increasing to 9.8% after 20 years. By contrast, 3.2% and 4.2% of surgically-treated men developed secondary pelvic malignancies over the same durations. There was no difference in deaths from secondary malignancies between the groups.
The strength of the association with bladder cancer in particular is “similar to that seen with smoking,” wrote the author of an accompanying editorial. Results from the study “should be considered when treating men with localized prostate cancer who have a long life expectancy,” the authors concluded.
Commentary from experts
“I do believe that this study reveals a dark truth about radiation for prostate cancer that has been long suspected,” says Dr. Anthony Zietman, a professor of radiation oncology at Harvard Medical School and Massachusetts General Hospital, and a member of the advisory and editorial board for the Harvard Medical School Guide to Prostate Diseases. “As the decades pass after radiation therapy of any kind — brachytherapy or external beam — the risk for radiation-induced malignancies rises.
“These malignancies are usually in adjacent organs like the bladder and rectum, or within the prostate itself. They may be very curable, and thus the survival rates are the same for radiation or surgically treated patients, but there is little doubt that, for these patients, they represent a ‘sting in the tail’ long after the radiation has been given and forgotten. This data certainly gives us pause when offering radiation to very young men with several decades of life expectancy ahead of them, and it also reminds us of the value of follow-up visits.”
“The fact that second cancers arise in the area where radiation was given is not surprising, but the magnitude of the long-term increases is concerning,” added Dr. Marc Garnick, the Gorman Brothers Professor of Medicine at Harvard Medical School and Beth Israel Deaconess Medical Center, and editor in chief of the Harvard Medical School Guide to Prostate Diseases. “There are other common and troublesome urinary side effects of brachytherapy — independent of second cancers — that patients should fully consider before selecting it as a treatment option. This is especially true given the availability of other convenient and similarly effective prostate cancer therapies.”
About the Author

Charlie Schmidt, Editor, Harvard Medical School Annual Report on Prostate Diseases
Charlie Schmidt is an award-winning freelance science writer based in Portland, Maine. In addition to writing for Harvard Health Publishing, Charlie has written for Science magazine, the Journal of the National Cancer Institute, Environmental Health Perspectives, … See Full Bio View all posts by Charlie Schmidt
About the Reviewer

Marc B. Garnick, MD, Editor in Chief, Harvard Medical School Annual Report on Prostate Diseases; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Marc B. Garnick is an internationally renowned expert in medical oncology and urologic cancer. A clinical professor of medicine at Harvard Medical School, he also maintains an active clinical practice at Beth Israel Deaconess Medical … See Full Bio View all posts by Marc B. Garnick, MD