
What is cognitive behavioral therapy?

Cognitive behavioral therapy (CBT) teaches people to challenge negative thought patterns and turn less often to unhelpful behaviors. These strategies can improve your mood and the way you respond to challenging situations: a flat tire, looming deadlines, family life ups and downs.
Yet there’s much more depth and nuance to this well-researched form of psychotherapy. It has proven effective for treating anxiety, depression, and other mental health conditions. Tailored versions of CBT can also help people cope with insomnia, chronic pain, and other nonpsychiatric conditions. And it can help in managing difficult life experiences, such as divorce or relationship problems.
What are the key components of CBT?
One important aspect of CBT relates to perspective, says psychologist Jennifer Burbridge, assistant director of the Cognitive Behavioral Therapy Program at Harvard-affiliated Massachusetts General Hospital.
“Therapists who practice CBT don’t see the problems or symptoms people describe as having one single cause, but rather as a combination of underlying causes,” she says. These include
- biological or genetic factors
- psychological issues (your thoughts, physical sensations, and behaviors)
- social factors (your environment and relationships).
Each of these factors contributes to — and helps maintain — the troublesome issues that might prompt you to seek therapy, she explains.
How does CBT describe our emotions?
Our emotions have three components: thoughts, physical sensations, and behaviors.
“Thoughts are what we say to ourselves, or 'self-talk,'” says Burbridge. Physical sensations are what we observe in our bodies when we experience an emotional situation: for example, when your heart rate rises in stressful circumstances. Behaviors are simply the things you do — or do not do. For instance, anxiety might prevent you from attending a social event.
All three components are interrelated and influence one another. That’s why CBT helps people to develop skills in each of them. “Think of it as a wellness class for your emotional health,” says Burbridge.
How long does CBT last?
CBT is a goal-oriented, short-term therapy. Typically it involves weekly, 50-minute sessions over 12 to 16 weeks. Intensive CBT may condense this schedule into sessions every weekday over one to three weeks.
Is CBT collaborative?
“When I first meet with someone, I’ll listen to what’s going on with them and start thinking about different strategies they might try,” Burbridge says. But CBT is a collaborative process that involves homework on the patient’s part.
What might that mean for you? Often, a first assignment involves self-monitoring, noting whether there are certain things, events, or times of day that trigger your symptoms. Future sessions focus on fine-tuning approaches to elicit helpful, adaptive self-talk, and problem-solving any obstacles that might prevent progress.
Certain thinking patterns are often associated with anxiety or depression, says Burbridge. Therapists help people recognize these patterns and then work with patients to find broader, more flexible ways to cope with difficult situations.
“We’re cognitive creatures with big frontal lobes that help us analyze situations and solve problems. That’s useful in some situations. But at other times, when you’re trying to manage your emotions, it may be better to pause and acknowledge and accept your discomfort,” says Burbridge.
Which CBT tools and strategies can help?
That particular skill — paying attention in the present moment without judgement, or mindfulness — is a common CBT tool. Another strategy that’s helpful for anxiety, known as exposure or desensitization, involves facing your fears directly.
“People avoid things that make them nervous or scared, which reinforces the fear,” says Burbridge. With small steps, you gradually expose yourself to the scary situation. Each step provides learning opportunities — for example, maybe you realize that the situation wasn’t as scary as you though it would be.
By trying new things instead of avoiding them, you begin to change your thought patterns. These more adaptive thinking patterns then make it more likely you will try new or challenging experiences in the future, thereby increasing your self-confidence.
How does CBT work?
Brain imaging research suggests conditions like depression or anxiety change patterns of activity in certain parts of the brain. One way CBT may help address this is by modifying nerve pathways involved in fear responses, or by establishing new connections between key parts of the brain.
A 2022 review focused on 13 brain imaging studies of people treated with CBT. The analysis suggested CBT may alter activity in the prefrontal cortex (often called the “personality center”) and the precuneus (which is involved in memory, integrating perceptions of the environment, mental imagery, and pain response).
Who might benefit from CBT?
CBT is appropriate for people of all different ages. This can range from children as young as 3 years — in tandem with parents or caregivers — to octogenarians. In addition to treating anxiety and depression, CBT is also effective for
- eating disorders
- substance abuse
- personality disorders
- attention deficit hyperactivity disorder (ADHD)
- obsessive compulsive disorder (OCD).
Additional evidence shows CBT may help people with different health issues, including irritable bowel syndrome, chronic fatigue syndrome, fibromyalgia, insomnia, migraines, and other chronic pain conditions. The therapy may also benefit people with cancer, epilepsy, HIV, diabetes, and heart disease.
“Many medical conditions can limit your activities. CBT can help you adjust to your diagnosis, cope with the new challenges, and still live a meaningful life, despite the limitations,” says Burbridge.
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
Julie Corliss is the executive editor of the Harvard Heart Letter. Before working at Harvard, she was a medical writer and editor at HealthNews, a consumer newsletter affiliated with The New England Journal of Medicine. She … See Full Bio View all posts by Julie Corliss
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

Ever read your medical record? Here’s why you should

Do you ever read the notes written by your doctor or health practitioner during a medical visit? If not, you might want to check them out. Usually, these medical notes are full of helpful insights about your health and reminders of recommendations discussed. And there’s medicalese, of course: hard-to-pronounce illnesses, medications, and technical terms.
But you may be surprised to see incorrect information or unexpected language, tone, or even innuendo. Was your past medical history really that “unremarkable”? Did you actually “deny” drinking alcohol? Did the note describe you as “unreliable”?
Here’s how to decipher unfamiliar lingo, understand some surprising descriptions, and flag any errors you find.
What’s in a medical note?
A standard medical note has several sections. These include
- a description of current symptoms
- past medical problems
- a list of medications taken
- family medical history
- social habits such as smoking, drinking alcohol, or drug use
- details of the physical examination
- test results
- a discussion of the big picture, along with recommendations for further evaluation or treatment.
Notes tend to be more complete for a new patient or annual exam. Follow-up notes may not cover all of these points.
What’s potentially confusing about medical notes?
Most medical notes aren’t written using plain language because they aren’t intended primarily for a nonmedical audience. So it’s common to run across:
- Medical jargon: You had an upset stomach and a fever. Doctors may say “dyspepsia” (upset stomach) and “febrile” (fever).
- Complicated disease names: Ever heard of “multicentric reticulohistiocytosis” or “progressive multifocal leukoencephalopathy?” These are just two of thousands of examples.
- Use of common language in uncommon ways: For example, your medical history might be called “unremarkable” and test results called "within normal limits” rather than “normal.”
- Abbreviations: You might see “VSS” and “RRR,” meaning “vital signs stable” with a pulse that has a “regular rate and rhythm.”
If you’re having trouble deciphering a note or understanding your health issues, tests, and recommendations, check in with your doctor’s office for clarifications. The more you understand about your health and your options for care, the better.
What if a medical note is incorrect?
Minor errors in medical notes are not rare: maybe you had your tonsils removed 30 years ago, not 10 years ago. But there can be more important errors: stating that arthritis in your left knee is severe when it’s actually the right knee that’s severe could lead to having x-rays (or even surgery!) on the wrong side. And not properly recording a family history of cancer or heart disease could mean missing out on timely screening tests or preventive treatments.
In an era of ever-increasing time pressure, use of voice recognition software, electronic record templates, drop-down menus, and ability to copy and paste text, it’s easier than ever for health care providers to make (and perpetuate) errors in the medical record.
If you do see an important error that could affect your health, ask your provider to amend it.
What if the language in a medical note seems offensive?
Numerous studies have highlighted the problem of stigmatizing language in medical notes that can leave people feeling judged or offended. Negative attitudes can affect the quality of our health care and willingness to seek care, and can also widen health disparities. One study linked stigmatizing language to higher rates of medical errors. Of note, this study found higher rates of stigmatizing language and medical error among black patients.
Examples include:
- Depersonalization: A note might describe a patient as “a drug abusing addict” rather than a person struggling with drug addiction.
- Insulting or inappropriate descriptors: Notes might contain subjective descriptions that paint the patient in an unflattering light without providing context. For example, the note might say “the patient is unkempt and is drug-seeking” rather than “the patient is experiencing homelessness and has severe, chronic pain.” If a person’s recall of medical events from the past is hazy, they may be called “unreliable.”
- Dismissiveness: A medical note may suggest a symptom is not real or is exaggerated, rather than taking the complaint seriously.
- An untrusting tone: Language such as “she claims she never drinks” or “he denies alcohol use” may suggest mistrust by the physician.
Why might this happen, anyway?
How does such language make its way into medical notes? (To be clear, these possible explanations are not justifications.)
- Tradition and training: Medical trainees, like other learners, tend to follow the lead of their mentors. So if stigmatizing language is used by an instructor, trainees may do the same.
- Time pressure: With medical documentation (as in most everything else), mistakes are more common if you’re rushing.
- Bias: Like everyone else, doctors have biases, including ones they aren’t aware of. How we are taught to think about people — by family, by society — can spill over into every area of life, including work.
- Frustration: Doctors may feel frustrated by patients who don’t follow their recommendations. That frustration can be reflected in their medical notes. For example, a note may say, “As expected, the patient’s blood sugar is high; he is still not checking his blood sugar or following the diet recommended by his nutritionist.”
If the language in a note is confusing or bothersome, ask about it. The Open Notes movement and federal legislation have given most of us much better access to our medical records. This has worthy goals — greater transparency and better communication with people about their medical care — and unintended consequences.
Is changing language in notes that health practitioners once shared mainly with each other a positive consequence? Mostly. Yet some doctors worry that notes will become less specific, accurate, or useful since they may leave out information that might upset a patient.
The bottom line
I encourage you to read your health providers’ notes about your care. If there is a substantial error or something you find confusing or objectionable, ask about it. By the way, a signed medical note cannot usually be revised. However, your doctor can make clarifications or correct mistakes in an addendum at the end of the note.
As more and more patients read their medical notes, it’s likely that health providers will be more conscientious about the language they use. So, wide access to medical notes may improve not only people’s understanding of their health, but also the quality of notes over time.
It's worth remembering that the medical note is not the most important thing that happens during a visit to your doctor. A great note isn’t the same as great care, and vice versa. Still, your medical notes can be a valuable source of health information that differs from all others, including trusted health sites and social media: they’re written by your doctor and they’re all about you.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD

Dog bites: How to prevent or treat them
 Each year, more than 4.5 million dog bites occur in the United States. Despite what you might assume, most of these incidents don’t happen when an unfamiliar dog attacks someone in a park or another outdoor location. Instead, most dog bites are inflicted by a pet dog in a home.
Each year, more than 4.5 million dog bites occur in the United States. Despite what you might assume, most of these incidents don’t happen when an unfamiliar dog attacks someone in a park or another outdoor location. Instead, most dog bites are inflicted by a pet dog in a home.
Here’s advice for avoiding these upsetting and potentially serious injuries — and the steps you should take if you sustain a dog bite.
Why do dog bites happen?
Some dog bites happen by accident when people wrestle or play tug-of-war with their dog. But most of the time, dogs bite people as a reaction to feeling stressed, threatened, scared, or startled, according to the American Veterinary Medical Association (AVMA). More than half of dog bites occur in children, and they’re far more likely to be seriously injured than adults.
“People don’t always heed the behavioral signals that a dog is uncomfortable,” says Dr. Christopher Baugh, associate professor of emergency medicine at Harvard Medical School. For example, some dogs are highly territorial and will bark, growl, snap, and lunge if outsiders enter their space — whether that’s an apartment, yard, or crate. Or dogs may exhibit resource guarding, which shows up as anxious, aggressive behavior around food, toys, or beds.
“These situations can be high-risk, and children in particular have less awareness of that risk,” says Dr. Baugh, who has children and two mixed-breed rescue dogs, Harley and Roxi.
What can you do to prevent dog bites?
Any dog — even a sweet, cuddly dog — can bite if provoked, according to the AVMA. Never leave young children alone with a dog without adult supervision. And teach children to never disturb a dog while it’s eating, sleeping, or caring for puppies.
In a study of 321 facial dog bites treated at Harvard-affiliated Massachusetts General Hospital over a 20-year period, 88% of the bites were from known dogs. Most were in adults and occurred after playing with the dog, feeding the dog, and placing their face close to the dog. However, the hand (usually a person’s dominant hand) is probably the most common location for a dog bite in an adult, says Dr. Baugh.
Other tips from the CDC to prevent dog bites include the following:
- Always ask a dog’s owner if it’s okay to pet their dog, even if the dog appears friendly.
- Make sure the dog sees and sniffs you before reaching out to pet it.
- Don’t pet a dog that seems to be hiding, scared, sick, or angry.
What if an unfamiliar dog approaches you? Remain calm and still, avoiding eye contact with the dog. Stand with the side of your body facing the dog and say “no” or “go home” in firm, deep voice. Wait for the dog to retreat or move yourself slowly away.
What should you do if you’re bitten by a dog?
Clean the wound with mild soap and running water, then cover it with a clean bandage or cloth. Some online resources recommend applying an antibiotic ointment or cream. But these products are recommended only for people with clear evidence of an infection, such as redness, pus, pain, swelling, or warmth, according to the American Academy of Dermatology.
If the injury is serious — with a bite on the face, heavy bleeding, or a possible broken bone — go to the emergency room. That’s also a good idea if you’re bitten by an unknown or stray dog, in the rare event that you might need medicines to prevent rabies (rabies post-exposure prophylaxis).
“Often, people are shocked after being bit and will understandably focus all their attention on their wound,” says Dr. Baugh. The dog’s owner may check in to see if you’re okay, but then walk away. But you should get the person’s contact information and make sure the dog is vaccinated against rabies, he says.
Keep in mind that:
- Emergency rooms are often crowded with long waits, so an urgent care clinic is a good option if the injury doesn’t require immediate attention.
- Some wounds require stitches, ideally within 12 to 24 hours.
- The doctor may prescribe antibiotics to prevent possible infections, especially if you have health problems such as a weakened immune system or diabetes.
- You may also need a tetanus booster if you haven’t had one in the past 10 years. If your vaccine history isn’t available or you can’t remember, you’ll get a tetanus booster just in case.
What if a dog bite is less serious?
Let’s say you have a less serious bite from a family dog known to have a current rabies vaccine. Bites that don’t require stitches can be cleaned with mild soap and running water, then evaluated by your regular health care provider. They may tell you to simply monitor the wound for signs of infection.
“Doctors are trying to be more thoughtful about prescribing antibiotics and limit their use in low-risk situations, because overuse contributes to antibiotic resistance and exposes people to potential side effects without any benefit,” says Dr. Baugh.
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
Julie Corliss is the executive editor of the Harvard Heart Letter. Before working at Harvard, she was a medical writer and editor at HealthNews, a consumer newsletter affiliated with The New England Journal of Medicine. She … See Full Bio View all posts by Julie Corliss
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD
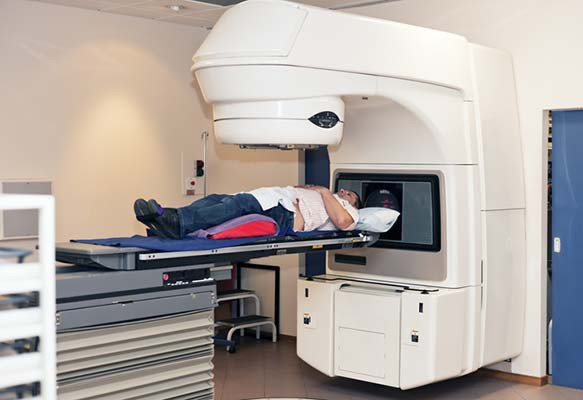
Prostate cancer: Brachytherapy linked to long-term risk of secondary malignancies

When cancer patients are treated with radiation, it’s possible that the therapy itself may cause new tumors to form in the body later. Radiation kills cancer cells by damaging their DNA, but if the treatments cause genetic damage to normal cells near the radiation target, there’s a small risk that these secondary malignancies may arise over time.
Just over 10 years ago, Canadian researchers set out to assess the risk of secondary malignancy among men with prostate cancer who were treated with a type of radiation called brachytherapy. Unlike radiation delivered from sources outside the body, brachytherapy is accomplished by implanting dozens of radioactive pellets, or “seeds,” directly into the tumor site. Those seeds, which are never removed, emit radiation at a dose that declines toward zero over the course of a year.
Brachytherapy has the advantage of convenience. Instead of traveling for repeat sessions of radiation, men need only one treatment, usually given in an outpatient setting. But brachytherapy is also falling out of favor, in part because newer types of external beam radiation deliver high-precision doses with fewer side effects.
Study methodology and results
The Canadian study compared rates of secondary malignancies in the pelvis among men treated either with brachytherapy or with surgery to remove the prostate. All the treatments took place in British Columbia between 1998 and 2000. The brachytherapy group included 2,418 men with an average age of 66, while the surgically-treated group contained 4,015 men whose average age was 62. Within that group, 2,643 men had been treated with surgery alone, and 1,372 men with surgery plus external beam radiation given later.
After median follow-ups of between 5.8 years (brachytherapy) and 6.4 years (surgery), the study team reported in 2014 that there was no difference in rates of secondary malignancies between the groups, or with cancer incidence in the general population.
But that’s no longer the case: In April 2024, the researchers published updated findings. This time, rates of new cancers in the pelvis — including the bladder and rectum — were higher in the brachytherapy group. Specifically, 6.4% of brachytherapy-treated men had secondary malignancies at 15 years of follow-up, increasing to 9.8% after 20 years. By contrast, 3.2% and 4.2% of surgically-treated men developed secondary pelvic malignancies over the same durations. There was no difference in deaths from secondary malignancies between the groups.
The strength of the association with bladder cancer in particular is “similar to that seen with smoking,” wrote the author of an accompanying editorial. Results from the study “should be considered when treating men with localized prostate cancer who have a long life expectancy,” the authors concluded.
Commentary from experts
“I do believe that this study reveals a dark truth about radiation for prostate cancer that has been long suspected,” says Dr. Anthony Zietman, a professor of radiation oncology at Harvard Medical School and Massachusetts General Hospital, and a member of the advisory and editorial board for the Harvard Medical School Guide to Prostate Diseases. “As the decades pass after radiation therapy of any kind — brachytherapy or external beam — the risk for radiation-induced malignancies rises.
“These malignancies are usually in adjacent organs like the bladder and rectum, or within the prostate itself. They may be very curable, and thus the survival rates are the same for radiation or surgically treated patients, but there is little doubt that, for these patients, they represent a ‘sting in the tail’ long after the radiation has been given and forgotten. This data certainly gives us pause when offering radiation to very young men with several decades of life expectancy ahead of them, and it also reminds us of the value of follow-up visits.”
“The fact that second cancers arise in the area where radiation was given is not surprising, but the magnitude of the long-term increases is concerning,” added Dr. Marc Garnick, the Gorman Brothers Professor of Medicine at Harvard Medical School and Beth Israel Deaconess Medical Center, and editor in chief of the Harvard Medical School Guide to Prostate Diseases. “There are other common and troublesome urinary side effects of brachytherapy — independent of second cancers — that patients should fully consider before selecting it as a treatment option. This is especially true given the availability of other convenient and similarly effective prostate cancer therapies.”
About the Author

Charlie Schmidt, Editor, Harvard Medical School Annual Report on Prostate Diseases
Charlie Schmidt is an award-winning freelance science writer based in Portland, Maine. In addition to writing for Harvard Health Publishing, Charlie has written for Science magazine, the Journal of the National Cancer Institute, Environmental Health Perspectives, … See Full Bio View all posts by Charlie Schmidt
About the Reviewer

Marc B. Garnick, MD, Editor in Chief, Harvard Medical School Annual Report on Prostate Diseases; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Marc B. Garnick is an internationally renowned expert in medical oncology and urologic cancer. A clinical professor of medicine at Harvard Medical School, he also maintains an active clinical practice at Beth Israel Deaconess Medical … See Full Bio View all posts by Marc B. Garnick, MD

Ultra-processed foods? Just say no

Americans love their ultra-processed foods, whether they come as cereal (like Cap’n Crunch, a favorite of mine as a kid), snack foods (like Cheetos), entr’es (like hot dogs), or desserts (like Twinkies). Sure, loading your plate with vegetables, fruits, fish, healthful oils, and grains in a Mediterranean-style diet boosts heart and brain health. But if you also eat some ultra-processed foods, is that bad for your brain health?
What to know about this new study
A new study appears to deliver resounding yes: eating ultra-processed foods is linked to a greater risk of cognitive impairment and strokes.
This well-designed observational study examined data from the REGARDS (REasons for Geographic And Racial Differences in Stroke) project, a longitudinal study of non-Hispanic Black and white Americans ages 45 years and older. Study participants were initially enrolled between 2003 and 2007 and were given a number of questionnaires evaluating health, diet, exercise, body mass index, education, income, alcohol use, mood, and other factors. In addition, tests of memory and language were administered at regular intervals.
To examine the risk of stroke and cognitive impairment, data from 20,243 and 14,175 participants, respectively, were found usable based on the quality of the information from the questionnaires and tests. Approximately one-third of the sample identified as Black and the majority of the remaining two-thirds identified as white.
The results of the study
- According to the authors’ analysis, increasing the intake of ultra-processed foods by just 10% was associated with a significantly greater risk of cognitive impairment and stroke.
- Intake of unprocessed or minimally processed foods was associated with a lower risk of cognitive impairment.
- The effect of ultra-processed foods on stroke risk was greater for individuals who identified as Black compared to individuals who identified as white.
Study participants who reported following a healthy diet (like a Mediterranean, DASH, or MIND diet) and consumed minimal ultra-processed foods appeared to maintain better brain health compared to those who followed similar healthy diets but had more ultra-processed foods.
Why might ultra-processed foods be bad for your brain?
Here are some biologically plausible reasons:
- UPFs are generally composed of processed carbohydrates that are very quickly broken down into simple sugars, equivalent to eating lots of candy. These sugar loads cause spikes of insulin, which can alter normal brain cell function.
- Eating ultra-processed foods is associated with a higher risk of metabolic syndrome and obesity, well-established conditions linked to high blood pressure, abnormal blood lipid levels, and type 2 diabetes.
- There are unhealthy additives in ultra-processed foods to change the texture, color, sweetness, or flavor. These additives disrupt the microbiome in the gut and can lead to gut inflammation that can cause
- the production of microbiome-produced metabolites that can affect brain function (such as short-chain fatty acids and lipopolysaccharides)
- leaky gut, allowing toxins and inflammatory molecules to enter the bloodstream and go to the brain
- altered neurotransmitter function (such as serotonin) that can impact mood and cognition directly
- increased cortisol levels that mimic being under chronic stress, which can directly impact hippocampal and frontal lobe function, affecting memory and executive function performance, respectively
- an increased risk for Alzheimer’s, Parkinson’s, and other neurodegenerative diseases due to inflammatory molecules traveling from the gut to the brain.
- Because ultra-processed foods have poor nutritional value, people will often be hungry shortly after eating them, leading to overeating and its consequences.
The take-home message
Avoid processed foods, which can include chips and other snack foods, industrial breads and pastries, packaged sweets and candy, sugar-sweetened and diet sodas, instant noodles and soups, ready-to-eat meals and frozen dinners, and processed meats such as hot dogs and bologna. Eat unprocessed or minimally processed foods, which — when combined with a healthy Mediterranean menu of foods — include fish, olive oil, avocados, whole fruits and vegetables, nuts and beans, and whole grains.
About the Author

Andrew E. Budson, MD, Contributor; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Andrew E. Budson is chief of cognitive & behavioral neurology at the Veterans Affairs Boston Healthcare System, lecturer in neurology at Harvard Medical School, and chair of the Science of Learning Innovation Group at the … See Full Bio View all posts by Andrew E. Budson, MD

Life can be challenging: Build your own resilience plan

Nantucket, a beautiful, 14-mile-long island off the coast of Massachusetts, has a 40-point resiliency plan to help withstand the buffeting seas surrounding it as climate change takes a toll. Perhaps we can all benefit from creating individual resilience plans to help handle the big and small issues that erode our sense of well-being. But what is resilience and how do you cultivate it?
What is resilience?
Resilience is a psychological response that helps you adapt to life’s difficulties and seek a path forward through challenges.
“It’s a flexible mindset that helps you adapt, think critically, and stay focused on your values and what matters most,” says Luana Marques, an associate professor of psychiatry at Harvard Medical School.
While everyone has the ability to be resilient, your capacity for resilience can take a beating over time from chronic stress, perhaps from financial instability or staying in a job you dislike. The longer you’re in that situation, the harder it becomes to cope with it.
Fortunately, it’s possible to cultivate resilience. To do so, it helps to exercise resiliency skills as often as possible, even for minor stressors. Marques recommends the following strategies.
Shift your thoughts
In stressful situations, try to balance out your thoughts by adopting a broader perspective. “This will help you stop using the emotional part of your brain and start using the thinking part of your brain. For example, if you’re asking for a raise and your brain says you won’t get it, think about the things you’ve done in your job that are worthy of a raise. You’ll slow down the emotional response and shift your mindset from anxious to action,” Marques says.
Approach what you want
“When you’re anxious, stressed, or burned out, you tend to avoid things that make you uncomfortable. That can make you feel stuck,” Marques says. “What you need to do is get out of your comfort zone and take a step toward the thing you want, in spite of fear.”
For example: If you’re afraid of giving a presentation, create a PowerPoint and practice it with colleagues. If you’re having conflict at home, don’t walk away from your partner — schedule time to talk about what’s making you upset.
Align actions with your values
“Stress happens when your actions are not aligned with your values — the things that matter most to you or bring you joy. For example, you might feel stressed if you care most about your family but can’t be there for dinner, or care most about your health but drink a lot,” Marques says.
She suggests that you identify your top three values and make sure your daily actions align with them. If being with family is one of the three, make your time with them a priority — perhaps find a way to join them for a daily meal. If you get joy from a clean house, make daily tidying a priority.
Tips for success
Practice the shift, approach, and align strategies throughout the week. “One trick I use is looking at my calendar on Sunday and checking if my actions for the week are aligned with my values. If they aren’t, I try to change things around,” Marques says.
It’s also important to live as healthy a lifestyle as possible, which will help keep your brain functioning at its best.
Healthy lifestyle habits include:
- getting seven to nine hours of sleep per night
- following a healthy diet, such as a Mediterranean-style diet
- aiming for at least 150 minutes of moderate-intensity activities (such as brisk walking) each week — and adding on strength training at least twice a week
- if you drink alcohol, limiting yourself to no more than one drink per day for women and two drinks per day for men
- not smoking
- staying socially connected, whether in person, by phone or video calls, social media, or even text messages.
Need resilience training?
Even the best athletes have coaches, and you might benefit from resilience training.
Consider taking an online course, such as this one developed by Luana Marques. Or maybe turn to a therapist online or in person for help. Look for someone who specializes in cognitive behavioral therapy, which guides you to redirect negative thoughts to positive or productive ones.
Just don’t put off building resilience. Practicing as you face day-to-day stresses will help you learn skills to help navigate when dark clouds roll in and seas get rough.
About the Author

Heidi Godman, Executive Editor, Harvard Health Letter
Heidi Godman is the executive editor of the Harvard Health Letter. Before coming to the Health Letter, she was an award-winning television news anchor and medical reporter for 25 years. Heidi was named a journalism fellow … See Full Bio View all posts by Heidi Godman
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

Is there a good side to drug side effects?

Drug side effects are common, and often quite troublesome.
Major side effects, such as severe or even life-threatening allergic reactions, require immediate treatment and discontinuation of the drug. More minor symptoms may be tolerable when weighed against drug benefits. And sometimes, these go away on their own as the body gets used to the drug.
But there’s another type of side effect you hear much less about: ones that are beneficial. Though uncommon, they’re worth keeping in mind when you’re starting a new medicine.
Aren’t all side effects bad?
The term side effect is usually assumed to be a bad thing. And that’s typically true. But that leaves out the “good” side effects. Relatively little is published on this, so it’s not clear how common they are. But four notable examples include:
- Minoxidil (Rogaine, Gainextra, other brands). Developed in the 1970s for high blood pressure, this drug also increased hair growth in study subjects. What was initially considered a bothersome side effect eventually became its primary use: topical forms of this drug are commonly used to treat hair loss.
- Diphenhydramine (Benadryl or generic versions). This common treatment for allergic conditions has the side effect of drowsiness. For adults with allergy issues and trouble sleeping, the sedative effect can be helpful. Regular, long-term use of diphenhydramine is not recommended, as it may increase the risk of dementia.
- Sildenafil (Viagra or generic versions). Originally developed as a treatment for high blood pressure and angina, it didn’t take long for male users to realize the drug could trigger erections within 30 to 60 minutes. The makers of sildenafil recognized that under the right circumstances, this could be a highly beneficial side effect. In 1998 it was approved as a treatment for erectile dysfunction.
- Semaglutide (Ozempic, Wegovy, Rybelsus). This drug was developed to treat diabetes, but early users noticed reduced appetite and significant weight loss. Now, several formulations of these related drugs are approved for diabetes and/or weight loss.
In the best study I’ve read on the topic, researchers found more than 450 reports of serendipitous beneficial effects of various drugs since 1991. And that may be an underestimation, since report forms did not specifically ask for or label this type of side effect, according to the study authors.
Silver linings: Repurposing and repackaging drugs
While the discovery of helpful drugs can arise unexpectedly, drug developers are increasingly using a more intentional approach: using side effect profiles to look for new uses.
For example:
- A drug reported to cause reduced sweating as a side effect may be effective for hyperhidrosis, a condition marked by excessive sweating.
- Drugs reported to cause low blood pressure as a side effect might be effective treatments for high blood pressure (hypertension).
- New treatments for breast cancer may include older medicines that have a similar side effect profile as known anti-cancer drugs.
The availability of large side effect registries has made this method of identifying drugs for repurposing a more realistic option. So, even negative side effects can have a silver lining.
Bad side effects and the nocebo effect
While side effects can be positive, most are not. Medication side effects are a common reason people give for not taking prescribed drugs regularly. And adverse reactions to medicines prompt up to 8% of hospital admissions, according to one analysis.
To make matters worse, in some cases the expectation of side effects seems to make them more likely to occur. Called the nocebo effect, it increases the chances of experiencing a negative side effect and seems due, at least in part, to expectations. Contrast this with the placebo effect, where a sugar pill or another inactive treatment can lead to benefit.
The bottom line
Many people avoid taking medications because they fear possible side effects. That’s understandable. But not taking a medication can mean missing out on its benefits. And anticipation or expectation of side effects can increase the chances you’ll have them.
So, while it’s important to be aware of the most common side effects caused by the medicines you take, it’s also important not to overestimate your chances of experiencing them. And remember: there’s always a chance you’ll have a side effect you actually welcome.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD

Health care should improve your health, right?

It’s undeniable: modern medicine offers ever-expanding ways to heal and prevent disease. But it’s also true that health care can cause harm. One analysis found that about 6% of health care encounters caused preventable harm, leading to thousands of deaths each year. And it’s not just errors that cause trouble. Highly skilled health care providers can cause harm even when they do everything right.
So, how can you reduce your chances of being harmed? Understanding what you can do to lessen the possibility of harm and what’s beyond your control are good first steps.
Whatever happened to “first do no harm”?
Fortunately, it remains a central tenet of medical care. Yet our health care system is complex and fragmented. Each year new medications are added to an ever-growing list, and people live longer with more chronic medical conditions than happened in the past. So in one sense, the successes of modern medical care may contribute to the high rate of health care–related harm.
These harms are often due to our complicated system of health care rather than one individual’s mistake. Harm due to substandard or negligent care is known as medical malpractice. Both health care providers and health care systems have important roles to play in preventing harm to patients.
Are there harms that cannot be prevented?
An enormous volume of scientific research teaches the best ways to diagnose, treat, and prevent disease. Yet people can react to treatments in completely unpredictable ways.
For example, a common and standard antibiotic treatment (think penicillin) can cause anaphylaxis, a life-threatening allergic reaction. Fortunately this is rare, but unless you or your doctor know to avoid it due to past side effects, there’s always a small chance of a severe reaction.
Often less dramatic — yet also unpreventable — harms are:
- Medication side effects. Every medicine comes with potential side effects, such as nausea, sleepiness, or rash.
- Misdiagnosis. Because no one has perfect diagnostic skills, even the most skillful health care provider can be wrong. This can result in unnecessary or delayed treatment.
- Inaccurate test results. Just as no health care provider is perfect, no test is either. False-positive results (indicating an abnormality when none is present) and false-negative results (normal results when disease is present) are common in medical practice. These results can lead to unnecessary treatment or false reassurance.
Which harms can be prevented?
Preventable harms can be dramatically reduced. They’re often due to mistakes that can be caught and corrected. Frequently, it takes a combination of things to go wrong for harm to occur.
The “Swiss cheese model” is often applied here: imagine you’re a fly trying to travel through several chunks of Swiss cheese. (I know it’s an odd scenario, but stick with me here.) It’s impossible to fly through the cheese unless the holes line up just so.
Frequently in health care, several factors must line up for an error to sneak through — for example, giving a hospitalized patient a medication to which they are allergic. For that to happen, the wrong drug has to get past the prescribing doctor, the computerized ordering system, the hospital pharmacist, the nurse giving the medication, and the patient. That’s a lot of layers, so most often an error like this will be caught.
What can you do to avoid preventable harms?
Where do you fit in? In these three scenarios, here’s what you can do to avoid preventable harms.
The problem: Taking medicines you no longer need or more medicines than necessary.
It might not seem like a big deal to keep taking a medicine if it isn’t causing any problems. But all medicines can cause side effects that you’d do better to avoid if you can safely stop taking it or reduce the dose. Plus, harmful interactions can occur if another medicine is added to your list.
What you can do: Make sure you know why you need to take each of your medicines. Ask the providers who prescribe each medicine if it is still necessary to take it or if the dose can be safely reduced. Reducing a dose may reduce the risk of side effects and the likelihood of a harmful interaction.
The problem: Taking the wrong medicine or the wrong dose.
What you can do: At your doctors’ visits, take notes or bring a friend or family member to help you remember medicine instructions. Ask whether you can record the medication instructions your doctor gives you. Take a photo of the instructions you’re given in case you lose the written version. Double-check details of your medicine list with your pharmacist. And ask questions if you’re unsure about the medicines recommended to you.
The problem: Wrong site surgery.
Despite efforts to make this a “never error,” surgery on the wrong part of the body still happens.
What you can do: Make sure you and your surgeon agree on what part of your body and which side requires surgery. Most surgeons now mark the site with a special pen before surgery and ask you to confirm the site by adding your initials. (The ink doesn’t come off easily with skin cleaners applied prior to surgery).
Some of these tips require time or resources that aren’t available to everyone: you might not be able to bring another person with you to medical visits or have a recording device. But asking questions — and getting answers you understand — should be routine.
Where does malpractice fit in?
When the topic of health care–related harm comes up, malpractice may be the first thing you think about. Yet, the approximately 10,000 malpractice payments made each year in the US likely represent only a small portion of all harm related to health care.
There are several reasons for this, including:
- Even when negligent or substandard care occurs, it doesn’t always cause major or long-lasting harm that leads to a malpractice claim.
- Many people who could file malpractice suits elect not to, or may not even realize that they’ve experienced negligent care. Past studies suggest that less than 5% of people experiencing harm related to medical care file malpractice claims.
- Increasingly, health care providers and health care systems accept responsibility for preventable harm occurring on their watch, and offer compensation rather than waiting for a legal claim to be filed.
The bottom line
It’s an unfortunate reality that some harms due to health care are inevitable. But there are steps you can take to avoid preventable harm and lessen the chances that the person harmed is you.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD

One surprising effect of wildfires: Itchy, irritated skin

Are you finding yourself with itchy, irritated skin that you can’t stop scratching? Or have you wondered why your child’s eczema is suddenly worse and so hard to control? Mounting evidence suggests that wildfires, which are increasing in intensity and frequency, contribute to skin problems, including eczema flares.
What is eczema?
Eczema is a common chronic skin condition that affects about one in 10 people in the US. Its hallmarks are inflamed and dry, itchy patches of skin.
Atopic dermatitis is the most common type of eczema. It can run in families, often beginning in childhood. Typically, in the northern hemisphere, it grows worse during the winter season when the weather is cold and drying. Now some experts are seeing that pattern change. At Massachusetts General Hospital, for example, one dermatologist noted an unusual spike last summer in patients with flare-ups of eczema.
Why is eczema getting worse during summer?
In 2023, Canada experienced more than 6,000 wildfires that burned over 16 million hectares of land — an area larger than the entire state of Georgia. While far away from the devastation, the smoke reached across the US and more than 2,000 miles to Europe. Poor air quality from these distant wildfires caused eye and throat irritation and difficulty breathing.
In Boston, Dr. Arianne Shadi Kourosh, a dermatologist at Massachusetts General Hospital, also began to notice skin symptoms. Normally the dermatology clinics would see fewer than 20 people during a summer month for eczema, including atopic dermatitis. Suddenly that jumped to 160.
Looking back at summer month records from the last four years, her research showed that the number of visits for these skin complaints tracked with the severity of air pollution. These findings are consistent with other research noting an uptick in eczema flares and psoriasis flares associated with wildfire pollution. But why?
Researchers theorize that airborne pollutants might set off a cascade of effects within the body by activating an oxidative stress pathway. This damages the skin barrier and prompts an inflammatory response. This cascade also may play a role in the development of eczema.
What can you do to protect your skin?
Air pollutants in wildfire smoke may harm multiple organs — not just your heart and lungs, but also our skin, it seems. So, when outdoor air quality is bad due to wildfires, limiting your exposure can help reduce health risks. While we can say the same for industrial air pollution, wildfire pollution is likely worse due to its additional toxic particles.
- Seek help if you’re itching. Check with a dermatologist or your health team if you think wildfire smoke or other forms of air pollution might be affecting your skin.
- Check local air quality.AirNow.gov shares local, real-time air quality information and activity guidance. When recommended, stay indoors if possible. Shut doors, windows, and any outdoor air intake vents.
- Protect your skin. When you’re outdoors, wear a mineral-based sunscreen containing zinc or titanium. While most other sunscreens work through a chemical reaction to absorb the ultraviolet (UV) rays that damage skin, zinc and titanium sunscreens help by forming a barrier over skin that reflects off UV rays. The barrier also reduces the amount of pollutant particles getting to the skin to set off the inflammatory cascade. Wearing sunscreen protects against skin cancer, as well.
- Wash up. After coming back inside, cleansing your skin and applying a hypoallergenic moisturizer will help keep it healthy. If you do have eczema, choose cleansers and moisturizing products recommended by your dermatologist or health care provider.
About the Author

Wynne Armand, MD, Contributor
Dr. Wynne Armand is a physician at Massachusetts General Hospital (MGH), where she provides primary care; an assistant professor in medicine at Harvard Medical School; and associate director of the MGH Center for the Environment and … See Full Bio View all posts by Wynne Armand, MD

The cicadas are here: How’s your appetite?

You’ve probably heard the news: Cicadas are coming. Or — wait — they’re already here.
And are they ever! Due to an unusual overlap of the lifecycles of two types (or broods) of cicadas, trillions of cicadas are expected to emerge in the US by the end of June, especially in the Midwest.
If you’d like to see where they’ve already arrived, track them here. And if you’re wondering if this cicada-palooza could help with grocery bills, read on to decide for yourself how appealing and how safe snacking on cicadas is for you. The pros and cons could change your outlook on the impending swarm.
What to know about cicadas
Don’t worry, cicadas are largely harmless to humans. In fact, their appearance is welcome in places where people routinely snack on them as a low-cost source of calories and protein.
Estimates suggest up to two billion people regularly eat insects, especially in South and Central America, Asia, Africa, Australia, and New Zealand. Cicadas, when available, are among the most popular. And if you thought no one in the US eats cicadas, check out this video from a May 2024 baseball game.
Are you tempted to eat cicadas?
For plenty of people, cicadas aren’t the food of choice. Some people can’t get past the idea of eating insects as food. That’s understandable: after all, the culture in which we are raised has a powerful influence on what we consider acceptable in our diets. Something some Americans might find off-putting (such as eating snakes) is common in China and Southeast Asia. Meanwhile, people outside the US find aspects of the typical Western diet unappealing (such as root beer, peanut butter and jelly, and processed cheese).
But some people shouldn’t eat cicadas because it could be dangerous for them.
Why you should — or shouldn’t — eat cicadas
Eating cicadas is common in many parts of the world because they are
- nutritious: cicadas are low in fat and high in protein, including multiple essential amino acids
- inexpensive or free
- tasty (or so I’m told): descriptions of their flavor vary from nutty to citrusy to smoky and slightly crunchy.
In years when cicadas emerge, recipes for dishes containing cicadas emerge as well.
Then again, there are several good reasons to avoid making cicadas a part of your diet, including these:
- You just can’t get past the “ick” factor. Adventurous eaters may be willing to try or even embrace consuming cicadas, while others will be unable to view the idea as anything other than horrifying.
- You find the taste or consistency unappealing.
- You’re “cicada intolerant.” Some people get stomach upset, nausea, or diarrhea if they eat too many cicadas.
- You’re pregnant or breastfeeding, or are a young child. Concerns about even low levels of pesticides or other toxins in cicadas have led to recommendations that these groups not eat them. Doesn’t this suggest the rest of us should also steer clear? Well, thus far, at least, there’s no evidence that toxins in cicadas are causing health problems.
But there is one more very important entry on this list: people with a shellfish allergy should not eat cicadas. Odd, right?
The shellfish-cicada connection
Cicadas are biologically related to lobsters, shrimp, crabs, and other shellfish. So if you’re allergic to shellfish, you might also be allergic to cicadas. A particular protein called tropomyosin is responsible for the allergy. It’s found in shellfish as well as in many insects, including cicadas.
The allergic reaction occurs after eating the cicada. Just being around them or handling them won’t trigger a reaction.
Among people with a shellfish allergy, developing a reaction after eating cicadas could be a bigger problem than it seems: up to 10% of people have shellfish allergies and, as noted, insect consumption is common worldwide.
Is it okay for your dog or cat to eat cicadas?
Walking your dog after the emergence of cicadas can be a new and exciting experience for you and your pet! Dogs may chase after cicadas and eat them. Cats might, too, if given the chance. That can be a problem if your pet eats too many, as some will experience stomach upset or other digestive problems.
While the insects are considered harmless to dogs, the American Kennel Club says it’s best to steer them away from cicadas once they’ve eaten a few.
Which other insects trigger allergies?
While insect-related allergic reactions (think bee stings) and infections (like Lyme disease) are well known, the insect-food-allergy connection is a more recent discovery.
One recently recognized condition is the alpha-gal syndrome, in which a person bitten by certain ticks develops an allergy to meat. The name comes from a sugar called galactose-α-1,3-galactose (or alpha-gal) found in many types of meat including beef, lamb, pork, and rabbit. According to the CDC, up to 450,000 people in the US may have developed this condition since 2010.
There aren’t many rigorous studies of the overlap of insects and food allergies, so there are probably others awaiting discovery.
The bottom line
When it comes to eating cicadas, I’ll pass. It’s not because of the risks. I’ve never had a problem with shellfish, and for most people the health risks of eating cicadas seem quite small. It’s just unappealing to me, and I’m not a particularly adventurous eater.
But let’s go easy on those who do enjoy snacking on cicadas. Insects offer a good source of calories and protein. Just because eating them seems unusual in the US doesn’t make it wrong.
So, if you like to eat cicadas and have no shellfish allergy or other reason to avoid them, go for it! This may be a very good summer for you.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD